Peripheral Arterial Disease VS Chronic Venous Insufficiency, a comparison a lot of people want to know about. PAD and CVI are two different vascular conditions that are caused by different factors, lead to distinct symptoms, and require different treatment approaches. Moreover, understanding the distinct features between the two enhances and facilitates accurate diagnosis and treatments.
What is Peripheral Arterial Disease?
Peripheral Arterial Disease is commonly referred to as PAD. It is a vascular condition that causes problems in one’s arteries, impairing blood flow to the lower extremities like legs and even arms. In addition, the root cause can be stated as atherosclerosis, which is a condition marked by the buildup of plaque in arteries that restricts blood flow. Risk factors like smoking, high BP, high cholesterol levels, aging, genetics, and diabetes drive this condition.
What is Chronic Venous Insufficiency?
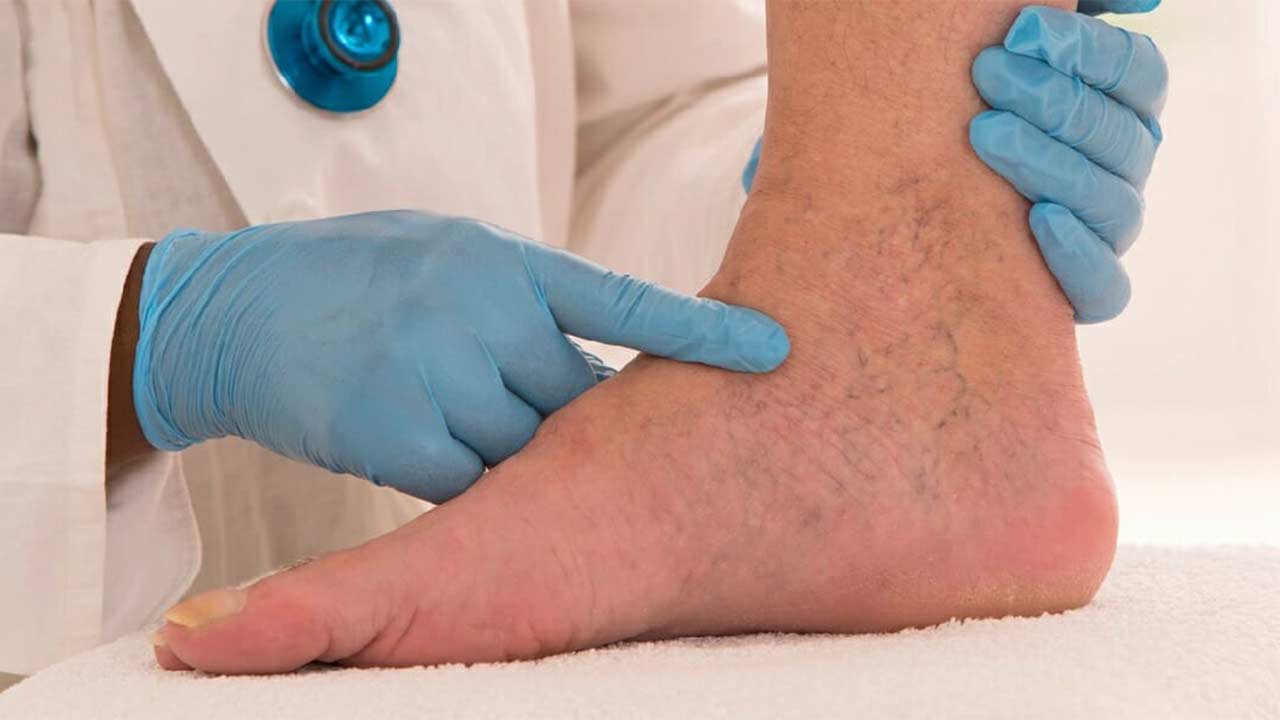
Chronic Venous Insufficiency is commonly known as CVI; this vascular disorder impacts veins’ inefficiency in transporting blood back to the heart. CVI is a result of factors like prolonged sitting or standing, obesity, family history, and genetics. As a result, a person experiencing this condition has a risk of developing blood clots in the deep veins.
Peripheral Arterial Disease VS Chronic Venous Insufficiency
PAD and CVI both have different symptoms, diagnostic approaches, and treatment strategies. Hence, the debate on peripheral arterial disease versus chronic venous insufficiency is quite detailed.
PAD Symptoms
PAD typically leads to symptoms like reduced blood flow, intermittent claudication (pain, cramping, and discomfort), numbness, weakness, coldness in the legs, etc. As a result, in extreme cases, PAD leads to critical conditions like non-healing wounds and limb amputation.
CVI Symptoms
CVI manifests symptoms like impaired venous return. Leg swelling, varicose veins, discomfort in legs, aching, discoloration of veins, leg ulcers, etc. are all results of CVI.
Diagnostic Approaches
PAD Diagnosis
Diagnosis of PAD involves non-invasive tests like ankle-brachial index (ABI) to compare blood pressure in the ankle and arm and Imaging studies like Doppler Ultrasound for detailed information about blood flow in arteries.
CVI Diagnosis
The diagnosis of CVI involves physical examination to assess symptoms physically and imaging studies like duplex ultrasound to visualize blood flow in veins and to identify abnormalities.
Treatment strategies for PAD & CVI
Peripheral Arterial Disease
PAD treatment focuses on preventing complications to improve blood flow. However, a person may make changes in their lifestyle by making regular exercise a part of their routine and increasing an intake of heart-healthy diet. Moreover, quitting smoking is crucial to treating PAD. In cases where PAD progresses to advanced stages, medical interventions like endovenous ablation or sclerotherapy become necessary.
Chronic Venous Insufficiency
CVI management aims to alleviate symptoms and improve blood circulation in the body. Compression stockings are commonly recommended to reduce swelling and discomfort. Furthermore, lifestyle changes, such as leg elevation and regular exercise, play a crucial role. Moreover, medical interventions like endovenous ablation or sclerotherapy may be employed to address specific venous issues.
Prognosis
- Peripheral Arterial Disease
- Critical limb ischemia
- Non-healing wounds
- Increased risk of cardiovascular events
Chronic Venous Insufficiency
- Venous Ulcers
- Skin changes
- Infections
- Reduced Quality of Life
Recognizing that peripheral artery disease (PAD) and chronic venous insufficiency (CVI) have different anatomical locations, causes, symptoms, and treatment approaches is crucial for ensuring accurate and timely diagnosis of both.